You are here:
- Procedures / ICL implantation
ICL Implantation
What is ICL implantation?
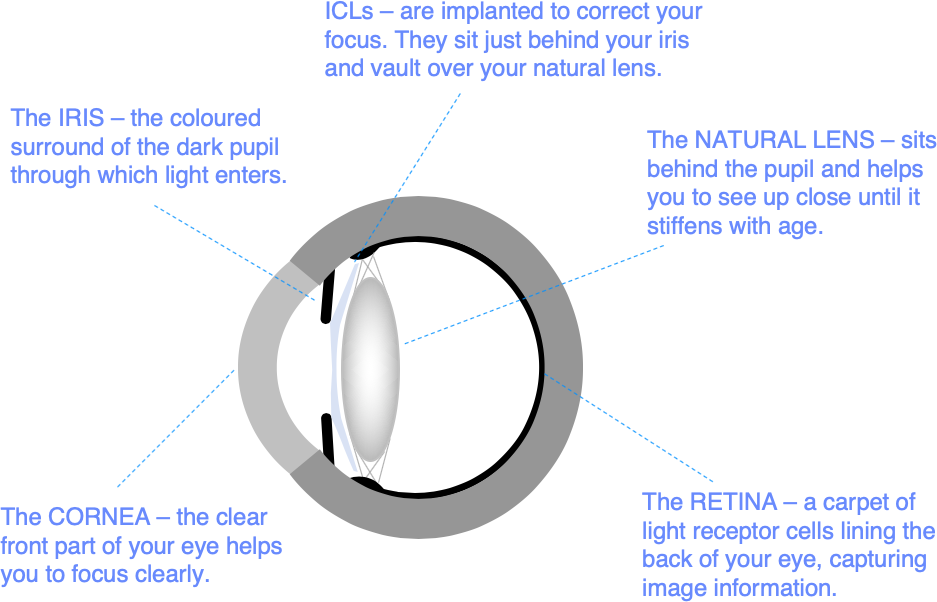
ICLs are soft flexible implants designed to sit just behind the pupil and in front of the natural lens – a bit like building your contact lenses into your eyes. You cannot see or feel ICLs after implantation, and you do not need to clean them.
ICL implantation is effective in treating high spectacle prescriptions, and is widely used to treat younger patients who are not suitable for laser eye surgery.
Over 1 million ICLs have been implanted since their introduction in 1992.
What are the benefits?
ICLs are highly effective at treating both high spectacle prescriptions and astigmatism. For most patients, vision after ICL surgery is similar to vision in contact lenses before surgery without the discomfort and limitations on activity.
Glasses may still be required for some activities after treatment, particularly reading in older patients, but these will be a low prescription and relatively inexpensive.
Over 95% of patients are satisfied with the outcome of surgery, and many describe it as life changing. Although ICL implantation is often bracketed with cosmetic surgery procedures, the benefits are mainly functional. It is designed to make you less dependent on glasses and contact lenses, helping you to lead an active lifestyle more easily.
Short sight and astigmatism normally stabilize in the late teens or early 20s, but natural prescription changes can occur at any stage in life. So, laser vision correction is sometimes needed to enhance distance vision in the years after ICL implantation.
Who is suitable for ICL implantation?
Young patients who are unsuitable for laser vision correction are often offered ICL implantation. This is because ICLs can correct a wider range of spectacle prescriptions than laser vision correction, and may be a safer option if you have pre-existing cornea or eye surface problems.
You need to be over 18 years of age and have a stable spectacle prescription. This is normally defined as no change greater than 0.5 units (0.5D) in the last 2 years.
The range of spectacle prescriptions that can be treated effectively with the ICL, is approximately:
- Up to -17.00D of myopia or short sight
- Up to +10.00D of hyperopia or long sight
- Up to ±4.50D of astigmatism
Supplementary laser vision correction or a different type of lens implant can be used to extend this range for suitable patients with very high prescriptions. Combination treatment with laser vision correction is sometimes called BIOPTICS.
You may not be suitable for ICL implantation if you have other problems with your eye health including cataracts, glaucoma, or recurrent inflammation in the eyes (uveitis). You also need to have enough room in the front of the eye to fit the ICL safely. This is normally determined by a scan of the eye at your initial consultation. We do not normally operate on patients while they are pregnant or breast feeding.
What are the alternatives?
Vision correction surgery alternatives
ICL implantation is one of three main categories of operations to correct vision. The other two are laser vision correction and refractive lens exchange (RLE).
Laser vision correction does not require a lens implant, and works by altering the curvature and focusing power of the front surface of the eye.
RLE is identical to modern cataract surgery, and works by replacing the natural lens with a lens implant.
Laser vision correction is generally preferred if you have a lower spectacle prescription. This is because there are very few longer-term risks associated with laser vision correction; whereas problems including cataract can occur many years after ICL implantation.
Older patients with a high spectacle prescription are more at risk of getting a cataract after ICL implantation, and they have already lost most of the flexibility of focus provided by the natural lens. So, after about 50 years of age, RLE is sometimes a better option if you are unsuitable for laser vision correction, particularly if you already have the beginnings of a cataract developing.
We will advise on your best treatment options after reviewing your test measurements and your eye health.
Alternative phakic intraocular lenses
ICLs are the most widely used lens implant in a category called phakic intraocular lenses (PIOLs). Any lens implanted to correct vision without removing your natural lens is called a PIOL. Different types of PIOL have a different safety profile. Most surgeons now prefer the ICL because it is easy to implant through a small entry into the eye and it has a very good long-term safety record. Similar PIOLs are becoming available from other manufacturers. These lenses are less costly than the ICL, but they are made from a different soft plastic material and, at this stage, we know less about their long-term safety. Sizing can be an issue for the ICL, and some ICLs need to be replaced soon after the initial operation. Lenses that clip onto the iris either side of the pupil called the Artisan or Verysise PIOL have been widely used in the past, and have the advantage that one size fits all. This type of PIOL is still the best choice for some patients, but annual eye health monitoring is required after implantation.
If an alternative PIOL would be your best option, we will talk this through with you before your surgery.
Continuing in glasses or contact lenses
ICL implantation is elective. This means you can choose to proceed with it at any time, or not at all. The alternative is staying in glasses or contact lenses.
Glasses are risk free but can be expensive and very limiting in terms of the range of activities, particularly sport, that you can participate in if you have a higher prescription.
Contact lenses provide good all-round vision. They do not mist over during sport and will help you to be more active; but they can be inconvenient when travelling, make water sports more difficult, and should not be worn whilst showering, swimming or during sleep. Contact lens wear is sometimes associated with eye surface discomfort, and may be complicated by sight threatening infection.
The risks and benefits of ICL implantation should be balanced against those for continued contact lens wear, since this is the main alternative for active people considering vision correction surgery.
How is ICL implantation performed?
We normally perform ICL implantation using eye-drop anaesthetic supplemented by an injection in the back of your hand to relax you if required. Anaesthetic may also be washed around the back of your eye to prevent excessive eye movement. A spring clip gently holding your eyelids apart allows you to blink safely during surgery.
We will be looking through a microscope to perform the surgery. You will be lying down under a surgical tent with fresh air coming in underneath. A sticky plastic drape covers the skin around the eye and sticks the eyelashes out of the way.
We now normally operate on both eyes in sequence on the same day. This helps to get your two eyes working together from day one, accelerating your visual recovery. If you would prefer to have one eye operated on at a time, please do not hesitate to discuss the pros and cons with us. The surgery typically takes about 20 minutes per eye. You can return home on the same day as surgery.
Strong pupil dilating drugs are given as drops or a using a pellet placed under the lower eyelid to prepare the eye for surgery.
Essential steps in ICL implantation surgery are:
- Entry points - formation of small self-sealing entry points in the front of the eye at the junction of the white of the eye and the cornea.
- ICL insertion - injection of the ICL and unfolding into position using a supporting gel to fill the front of the eye. Sometimes a small bypass drainage hole is formed in the iris at this point, but this additional stage is no longer required for newer (v4c) ICLs in myopic patients.
- Wash out and refilling - washout of the supporting gel and refilling with fluid and antibiotics.
What are the risks?
In all forms of eye surgery, problems can occur during the operation or afterwards in the healing period. Problems can result in permanent, serious loss of vision (vision worse than the driving standard in the affected eye that cannot be corrected with glasses or contact lenses). More commonly, problems can be corrected with changes in medication or additional surgery. Typically, these additional operations feel like the original surgery and have a similar recovery period.
Loss of vision
Permanent, serious loss of vision is very uncommon after ICL implantation. Causes include damage to the nerve at the back of the eye caused by a sudden rise in fluid pressure within the eye after surgery, and damage to the retina caused by infection or retinal detachment. Sudden pressure rises are much less common with the newer v4c and later ICLs used for treating myopic patients. The v4c and later ICLs allow natural fluid flow through the pupil and do not require a bypass drainage hole in the iris. If pressure rises do still occur, it is normally because of incomplete removal of supporting gel – a problem that can be fixed relatively easily with further washout. All patients with high levels of short sight have a higher risk of retinal detachment. This risk is not increased by ICL implantation, which does not involve surgery to the back compartment of the eye. Infection rates after ICL implantation are very low (approximately 1 in 6000). Complete loss of vision can occur after any operation involving the inside of the eye; but this is rare after ICL implantation.
Additional surgery
Cataracts may occur earlier in life than they would have done otherwise after ICL implantation. Cataract surgery can normally be combined with ICL removal if necessary, and substitution of a new lens implant during cataract surgery helps to minimize any additional requirement for glasses. In other words, ICL implantation does not stop you having successful cataract surgery or RLE later in life if this is required.
Statistical techniques are used to size ICL implants. The size prediction is sometimes wrong, and in approximately 1 case in 40, the ICL needs to be replaced with a lens of a different size in order to get the best fit in the eye. A minor rotation of the position of an ICL implant is also sometimes required after surgery to optimize the correction of astigmatism.
ICLs can be removed if they are causing problems. This usually means that your vision and eye health will be the same as it was before ICL implantation. But not all problems caused by ICLs can be corrected by removing them, and additional treatment may be required even after ICL removal.
ICL removal is uncommon unless you require cataract surgery or an ICL of a different size.
Risks of contact lens wear
Continuing in contact lenses is often the main alternative for people considering sight correction surgery. If you follow the right safety advice, contact lens wear is low risk; but approximately 1 in 3000 wearers each year will develop a serious corneal infection.
To minimize this risk, you should not swim or shower in contact lenses, and should not wash them in tap water. Sleeping in contact lenses, including those designed for overnight wear, increases the risk of infection significantly. Soft, daily disposable lenses are safer than non-disposable lenses.
What are the side effects?
Side effects are problems which most patients experience to some degree after surgery. They normally improve with time, but do not always resolve completely.
Vision
It is normal to experience some light scatter side effects in the early period after ICL implantation, particularly if you have treatment for a very high spectacle prescription. These can take a variety of forms including glare, halos, starbursts and ghost images. Increased flare from oncoming car headlights is a common symptom, and night driving may be difficult at first. Visual side effects are usually mild and improve within a few months. ICLs can be removed if visual side effects persist, but this is rarely required.
Eye comfort
Some eye surface discomfort is common in the early months after most forms of eye surgery. This is usually mild after ICL implantation, and highly variable – often affecting one eye more than the other. Treatment and prevention are based on making sure your eye surface is healthy before and after surgery. Lubricant eye drops can be helpful, and can be taken safely in addition to your other medication when required. For patients with a normal eye surface prior to surgery, lasting problems are unusual.
Eye appearance
Red blotches are often visible on the white of the eye after any form of eye surgery. These are called subconjunctival haemorrhages, and are caused by a small leak of blood under the mucous membrane covering the white part of eye wall. Although they can be quite unsightly, red blotches are temporary, and do not affect eye health; but they can take up to 6 weeks to go away completely.
Will ICL implantation affect my future eye health care?
If you develop a new eye health problem in later life, ICL implantation should not prevent you having successful treatment. Common eye health problems like glaucoma, diabetic retinopathy, and age-related macular degeneration can be monitored and treated as normal after ICL implantation.
Annual review with your local optometrist is normally recommended after ICL implantation to check on your eye health. This is particularly important if you have high myopia (you are very short sighted) before the surgery. This is because high myopia increases the risk of new problems like macular degeneration and glaucoma that may need early stage treatment to prevent permanent problems with vision. ICL implantation corrects vision, but does not change the risk of other eye health problems associated with extreme short sight.
How can I reduce the risk of problems?
Most patients have ICL implantation under local anaesthetic. You can eat and drink normally before surgery, and should take any regular medication as usual.
We work with an anaesthetist to monitor your health and optimize your comfort during surgery, administering sedation where necessary. Keep your breathing calm, stay as relaxed as you can, and try to keep your head still after we have positioned it comfortably for you.
You can help us apply the drape and stick your eyelashes out of the way by opening both your eyes wide at the beginning of surgery. You should clean off any make-up or moisturising cream before surgery to help the adhesive drape to stick properly. Blinking is no problem after the draping is complete. Just look straight up ahead to the bright operating light with both eyes open, but blink when you need to. Looking up to the bright microscope light helps to keep your eyes in the best position.
We will talk you through the procedure, encouraging you at every stage. Let him know if you feel any discomfort, and tell him if you need to cough, sneeze or take a break.
A clear plastic shield is sometimes taped over your eye at the end of surgery. For most patients, this is no longer required. Non-prescription sunglasses can be worn outdoors whilst the eyes are still light sensitive in the first few days after treatment. Do bring a pair with you to wear on the way home.
You can wash and shower normally from day one after surgery. We recommend no swimming for a week and no contact sports for a month. Non-contact sports such as gym and jogging can be resumed from day one after surgery. It is safe to start driving again when you can read a number plate at 20 yards with both eyes open and you are reasonably comfortable with your new vision. Typically, this is within a few days of surgery.
Set a smart phone reminder and use the antibiotic and anti-inflammatory drops as prescribed to help the eyes to heal. It is good to leave at least 2 minutes between different types of eye drop so that they each absorb well before the next drop is applied. If you miss the first time or you are not sure, applying a second eye drop is no problem.
Some variability of vision and comfort is normal in the early weeks after ICL implantation, and patience is required. But discomfort is usually mild, and vision normally recovers substantially within 2-3 days once the pupil dilating drugs have worn off.
You should contact us without delay if you have increasing pain, light sensitivity, redness, blur. You will be given Mr Allan’s mobile phone number for emergency contact after surgery. The practice management and the laser nursing team are also available for informal advice. The Eye Casualty Department at Moorfields Eye Hospital is open for emergency review 24 hours a day, 7 days a week.
You may not be aware of a problem that requires treatment in the healing phase. So, make sure you attend your review appointments even if your eyes feel good.
Appointments and enquiries
If you wish to arrange a preliminary consultation, please telephone Angelique Thomas on 020 7566 2156 or 07484 081815 (or from outside the UK +44 20 7566 2156 or +44 7484 081815) or email moorfields.ballan@nhs.net
Additional information
This information is adapted from Standardised Patient Information on Phakic Intraocular Lens Implantation published by the Royal College of Ophthalmologists. This information and can be downloaded here