You are here:
- Procedures / Refractive surgery
Laser refractive surgery
Laser refractive surgery is based on microscopic reshaping of the cornea to correct myopia, hypermetropia, and astigmatism. The excimer laser removes tissue with submicron precision and has been used to reshape the cornea in refractive surgery for the over 25 years. Technical progress during this period has been rapid, and night vision problems (glare/halo/starburst) associated with earlier procedures have largely been eliminated by modern laser delivery systems.
Wavefront scanning (aberrotometry)
Wavefront scanning aims to take account of optical aberrations in the eye in addition to myopia, hypermetropia, or astigmatism. These higher order aberrations are best understood by thinking of your spectacle prescription as an average of the focusing requirements for light rays entering the eye through different points on the eye surface.
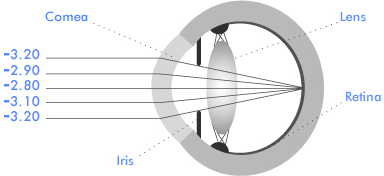
If your refraction is, for example, -3.00D, this may be an average of -2.80D for rays entering through the centre of the cornea and -3.20D for rays entering around the edge. A wavefront scan produces a map of the focusing requirement at each point. Information from this scan can be programmed into the excimer laser with the aim of reshaping the cornea to produce sharper vision than spectacles. Whilst this is a seductive concept, there are several practical difficulties. Limitations in the mathematics used to summarise wavefront-scanning information, and integral elements of refractive surgery, such as variation in individual healing responses, may have an unpredictable effect on the wavefront map.Current wavefront-guided laser treatments do not routinely produce better vision than spectacles and contact lenses, but they can help to improve overall visual quality and treatment accuracy in the right patients. Your suitability for wavefront-guided treatment will be discussed with you at your preliminary consultation.
The Schwind Amaris excimer laser
Because Moorfields Eye Hospital is a flagship location for manufacturers of laser equipment, we are able to select from all the leading excimer laser platforms and renew our equipment every 3 years. We are currently using the Schwind Amaris 1050RS excimer laser platform, which combines a proven clinical track record, with the best options for wavefront-guided laser treatment, improved eye tracking and the ability to create a more natural post-treatment corneal shape.
IntraLASIK
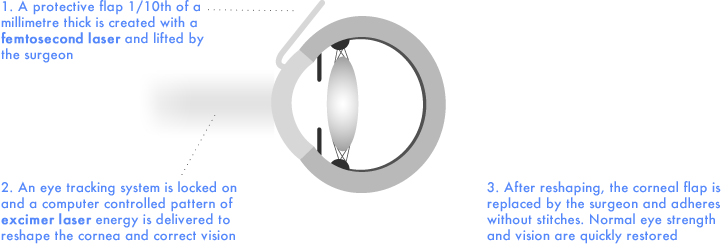
In modern LASIK, two lasers are used. First, a femtosecond laser is used to trace a 3D pattern of microscopic gas bubbles through the cornea to create a thin protective flap. The tissues beneath are then reshaped using a computer controlled excimer laser before the protective flap is replaced. In essence, the cornea is reshaped without surface damage. The femtosecond laser used at Moorfields Eye Hospital is the Intralase iFS. Noted for its precision and an excellent safety record, the intralase iFS is the most widely used femtosecond laser and is the industry standard for LASIK flap creation.
Why is a corneal flap used in LASIK?
Scarring responses throughout the body are driven by damage to surface tissues. Many plastic surgical procedures are based on the idea that if undamaged skin can be replaced or grafted onto a wound, scarring and tissue contraction will be minimized. LASIK is also based on this principle, using a thin protective corneal flap to avoid surface tissue damage and subsequent scarring responses. This provides a rapid, virtually painless recovery and fast stabilisation of the visual result.
Surface laser treatments
Reshaping beneath the corneal surface using a thin flap as in LASIK, rather than removing the corneal skin layer and reshaping the surface directly as in photorefractive keratectomy (PRK), has several advantages. LASIK is less painful than PRK, visual recovery is quicker, and the new corneal surface shape stabilises faster. Femtosecond lasers allow thinner flaps to be created with greater precision than earlier methods, expanding the range of patients that can be treated with LASIK. But surface laser treatments such as PRK, LASEK, Epi-LASIK or, most recently, TransPRK are often the safest option for patients with thinner corneas. Specialised surface laser treatments are also used increasingly commonly to correct visual problems arising after injury, infection or previous eye surgery.
TransPRK
The Schwind Amaris excimer laser system is programmed to remove the corneal skin layer quickly and painlessly from the central corneal surface prior to wavefront guided laser reshaping in transepithelial PRK (TransPRK or SmartSurfACE), the latest form of ‘no touch’ surface laser treatment. An anti-scarring drug, mitomycin C, is often applied to the corneal surface after laser reshaping to reduce haze (loss of corneal clarity) and regression (corneal shape changes during healing which can dilute the effect of treatment). A bandage contact lens is then placed to protect the operated area for a few days whilst the skin layer heals. Eye drops are used to minimise discomfort, but approximately 3-4 days in which the eyes are relatively sore, light sensitive and watery is normal. Vision returns over the next few weeks whilst the new skin layer remodels. Although recovery is slower after surface laser treatments than after LASIK, final visual results are normally equally good. Healing is typically 2 days faster after TransPRK than earlier surface laser treatments such as LASEK, and has recently been made faster still with the addition of a smoother tissues removal profile created by SmartPulse technology.
SMILE
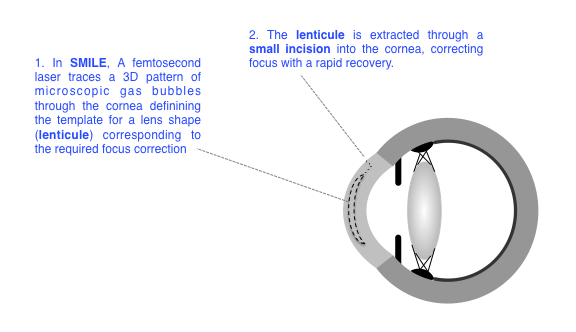
Small incision lenticule extraction (SMILE) is a new procedure, similar to LASIK, in which a femtosecond laser is used to define a corrective lens shape (lenticule) within the cornea. The lenticule is dissected free by the surgeon and removed through a small incision. Results are similar to those for LASIK. Visual recovery tends to be slightly slower, but recovery of surface comfort may be slightly quicker, and patients can return to contact sports at an early stage. SMILE is not currently compatible with wavefront-guided treatment, there is no eye image registration, and treatment is normally performed at a deeper level within the cornea than LASIK. Because of these possible disadvantages, we have not extended a recent clinical evaluation of the current version of SMILE at Moorfields.
Risks and Benefits
- Over 99% of wavefront LASIK patients starting with normal spectacle corrected vision and targeting good distance vision are able to see the driving standard or better without glasses after one treatment*. Results for surface laser treatments (Trans PRK) are similar.
- For patients who do not achieve a sharp focus after their initial laser treatment, enhancement treatment (retreatment) is highly effective in correcting significant residual refractive errors. Retreatment is carried out in approximately 3%* of cases overall. Retreatment is more common in patients with a higher starting prescription. There is no additional charge for retreatments carried out within 2 years of primary treatment (the need for any retreatment can normally be determined within 6 months of surgery).
- Common side effects such as mild dryness or light scatter during night driving normally resolve within 6 to 9 months of treatment. Permanent dry eye symptoms are rare in the absence of a pre-existing ocular surface problem, but may occur. Similarly, permanent unwanted visual side effects (including starburst, halo, glare, light scatter, ghost and double images) are rare and are often, but not always, improved by repeat laser treatment.
- Realistic expectations are important. Laser refractive surgery is highly effective in reducing spectacle dependence. At minimum, you should expect to be able to play sport and socialise comfortably without glasses after treatment; but some patients may still prefer to wear thin glasses for selected activities such as reading or night driving. This is especially likely for patients who are already in the reading glasses age group.
- Laser refractive surgery of any type does not routinely deliver above normal vision. Most patients have low-level residual refractive errors after surgery. These refractive errors are at a similar level to those normally found in non-spectacle wearers, and do not usually require retreatment.
- Progressive increasing reliance on reading glasses for near vision is normal from around age 45 for anyone with good uncorrected distance vision. This is not altered by laser refractive surgery, but effective treatment strategies are available to reduce near vision spectacle dependence for older patients.
- Vision should otherwise remain stable and good permanently after treatment. Your risk for developing other eye problems should not be altered. Natural variations in the distance spectacle prescription can occur at any age. These are usually small, but can be large enough to warrant further treatment in a small percentage of patients (less than 2% in the first 5 years after treatment).
- The overall complication rate for LASIK including retreatments is about 5%* (figures for surface treatments and SMILE are similar). Most problems are minor, and almost all complications can be corrected safely without affecting the final visual result. There is no charge for any additional consultations or treatment required for the correction of complications.
- Less than 1 in 1000 patients are left with significant scarring or corneal irregularity requiring a corneal graft or hard contact lens wear for visual rehabilitation. This level of risk is similar to the cumulative risk of corneal scarring resulting from infection in 5-10 years of contact lens wear.
- Most complications occur within 1 month of LASIK, TransPRK. The risk of long-term loss of corneal shape stability (keratectasia) after LASIK has recently been estimated at less than 1/1000 in a systematic review of the medical literature commissioned by NICE (the national institute of clinical excellence). Current patient selection strategies further reduce this risk. Medium term studies show significant benefits for using the anti-scarring drug MMC in selected patients undergoing surface laser treatment. MMC is associated with a low, but as yet unquantified, risk of long-term corneal damage. MMC is not used in LASIK.
- The benefits of refractive surgery are primarily functional. It is not a cosmetic procedure. Freedom from glasses and contact lenses will help you to enjoy sport, physical exercise, and a healthy active lifestyle. Refractive surgery is provided free to military personnel in the USA. 1 in 3 refractive surgeons who were previous spectacle wearers has already had refractive surgery performed on themselves. The commonest procedure chosen was LASIK.
(*These percentages are updated annually in accordance with audit of outcomes for patients treated by Bruce Allan at Moorfields Eye Hospital. Retreatment rates should not be compared between clinics without reference to the level of starting refractive error or the mean level of residual error treated in the group of patients studied. We often treat relatively complex prescriptions and work hard to ensure that our results remain in the front rank across all outcome measures in like-for-like comparisons with peer-reviewed benchmark data internationally)
Suitability for laser refractive surgery
Refractive errors typically do not stabilise until the late teens or early twenties. To be suitable for refractive surgery of any sort, you should be over 21 years of age with no change in your spectacle or contact lens prescription over the previous 2 years. The first step towards refractive surgery is obtaining an up to date spectacle prescription and records of any previous prescriptions over the last 2 years from your optician.
Laser refractive surgery is safest and most accurate in treating a defined range of refractive errors:
Myopia (-1.00 to -10.00D)
Astigmatism (up to ±6.00D)
Hypermetropia (+1.00 to +4.00D)
For refractive errors outside this range, implant based procedures such as intraocular collamer lens (ICL) implantation or refractive lens exchange (RLE) are normally preferred.
Laser refractive surgery may not be suitable if you have:
- Ocular surface disease. If you have dry eyes, active blepharitis, or allergic eye disease requiring regular drug treatment, corneal healing after laser refractive surgery may be adversely affected.
- Corneal disease or abnormality. You will be carefully screened to ensure that you do not have a condition called keratoconus prior to laser treatment. Mild forms of this corneal shape abnormality are relatively common, and can predispose to a poor result from laser refractive surgery.
- Cataracts. Cataract extraction presents an opportunity for refractive correction without laser surgery. An artificial lens is normally implanted in the eye during cataract surgery. The power of this lens can be chosen to correct any pre-existing refractive error. Patients over 50 years old commonly have early stage cataracts.
- Aspects of general health which might affect corneal healing. These include pregnancy, diabetes mellitus, autoimmune diseases, keloid scarring, and diseases requiring steroid medication by mouth. Small changes in your spectacle prescription may occur whilst you are pregnant or breast-feeding. For mothers with new babies, refractive surgery is normally postponed until 1 month has elapsed from the end of breast-feeding.
Planning treatment
Having scheduled your appointment for surgery, you will be given comprehensive instructions on preparation and aftercare appropriate to your procedure choice.
Time off work
Treatments are normally performed on a TUESDAY morning with initial postoperative review the following day. Office based work is usually no problem from the day after LASIK. For outdoor occupations and professional drivers work can normally be resumed by the MONDAY following treatment. We recommend 1 week off work for patients undergoing TransPRK.
Post operative consultation schedule
Patients are normally reviewed a minimum of twice after laser vision correction: at 1 day and 3 months after surgery, with additional review appointments as required. Liaison with a referring ophthalmologist for routine aftercare is usually possible for overseas patients. The minimum time in the UK for patients coming for treatment from overseas is 1 week.
Surgery in both eyes
Having both eyes corrected on the same day has considerable practical advantages, and is the preferred option for most patients undergoing laser refractive surgery. There are no safety advantages for delaying second eye surgery.
Enhanced range of focus (an option normally considered for patients over 40)
Electing to leave one eye relatively myopic (typically a 1.00D to 1.50D undercorrection) to assist near vision is the strategy of maximum spectacle independence for patients in the reading glasses age group (43 years and over). Glasses will still often be required to read fine print comfortably but spreading the focus between the eyes in this way typically delays the onset of spectacle dependence for reading until the mid fifties or later. Even then, spectacle dependence is decreased for common near vision tasks such as computer work and working with your hands. A spread of focus does not work for everyone, and may increase spectacle dependence for some distance vision tasks (typically night driving), but the compromise for distance vision is relatively small. Note that this is not conventional monovision, and the eyes still work together to produce the clearest image and judge distances. If you are in the reading glasses (presbyopic) age group, the pros and cons of alternative strategies for promoting overall spectacle independence will be discussed with you at your refractive surgical consultation.
The day of surgery
The surgery itself is relatively brief (under 30 minutes is required to treat both eyes), but some waiting time prior to surgery is usual, and further time is required for aftercare instruction and postoperative checks. Most patients spend 2-3 hours in hospital.
The surgery is not painful. You will feel touching around the eye, cold fluid on the eye surface, and gentle pressure on the eye at various stages during the surgery, but anaesthetic drops administered prior to surgery are highly effective in minimizing any discomfort.
What if I blink?
Adhesive drapes are used to tape the lashes out of the way and a gentle eyelid retainer is used to keep the lids open. Blinking is no problem. At the appropriate times, we will encourage you to look up at a flashing green fixation light – as if you are staring at a star on the horizon. The eye we are not operating on will be covered. You simply look up at the fixation light with both eyes open.
What if I move?
You can help the surgery to proceed quickly and accurately by gazing directly up at the flashing fixation light throughout the procedure, but involuntary eye movement is no problem. The Schwind Amaris system incorporates a sophisticated eye tracking mechanism that follows eye movements during treatment. Any movement outside the safe range will cause the laser to stop automatically. Mr Allan will be looking at your eyes through an operating microscope throughout, and can override the laser’s automatic cut out to stop and start the treatment as often as necessary to achieve the best result.
Mr Allan will talk you through the procedure and most patients comment that it is surprisingly easy. After the surgery, it is like looking through a watery fog. You are able to see enough to walk around without assistance, but the vision is not clear. Relatively clear vision normally returns within a few hours of LASIK treatment - you can typically see at the driving standard by the next day. Blurred vision is normal for up to 2 weeks after TransPRK but will normally catch up to the LASIK 4-6 weeks after treatment.
Appointments
If you wish to arrange a preliminary consultation, please telephone 020 7566 2156 or 07484 081815 (or from outside the UK +44 20 7566 2156 or +44 7484 081815) or email moorfields.ballan@nhs.net