You are here:
- Procedures / Introduction to cataract surgery
Introduction to cataract surgery and corneal transplantation
The focusing apparatus of the eye
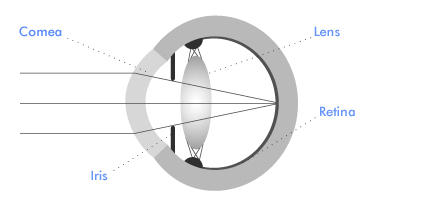
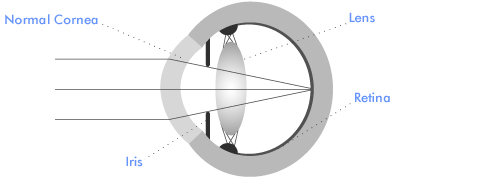
We see by forming an image on the retina - a carpet of light sensitive cells, each acting like a pixel on a computer screen, that lines the inside of the back of the eye. Images are focussed on the retina by the cornea (the clear part of the front of the eye) and the natural lens (suspended within the eye just behind the pupil). The aim of cataract and corneal surgery is to maintain a clear pathway for light to pass through the eye and focus on the retina.
Cataract surgery
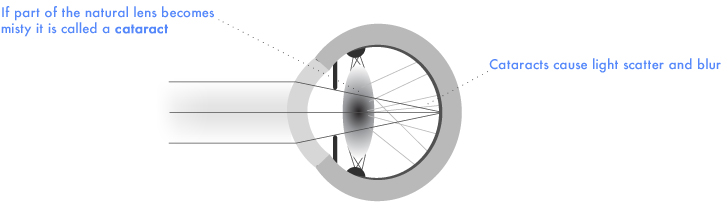
If you have been told you have a cataract, this means that part, or all, of your natural lens has become misty. Common symptoms of cataract are gradual loss of vision, increased light scatter from oncoming car headlights, and a shifting spectacle prescription. There are no proven drug or eyedrop treatments for cataract; but modern cataract surgery is low risk, painless, and highly effective in restoring good sight.
Cataract surgery involves replacing the misty natural lens with an intraocular lens implant (IOL), which restores a clear pathway for light and improves focus. A variety of IOL options, including multifocal and astigmatism correcting lens implants, and IOL selection strategies are available to help give greater freedom from spectacles after surgery. Endothelial Keratoplasty has several variations including DMEK, DSAEK, and DLEK.
Corneal transplantation
If the cornea becomes misty (as in Fuchs dystrophy) or has a poor focusing shape (as in keratoconus) you may require a corneal transplant. In modern corneal transplantation, the damaged layers of the cornea are replaced selectively with normal corneal tissue from an organ donor. Corneal transplantation is the commonest form of organ transplant. Over 5000 corneal transplants are performed each year in the UK. Unlike kidney or liver transplantation, most patients do not need drugs to suppress the immune system in order to prevent rejection reactions after a corneal transplant operation. Drop treatments are all that you would normally need. Most corneal transplants are successful, but revision surgery is commonly required in order to achieve the best result, and repeat transplantation may be necessary.
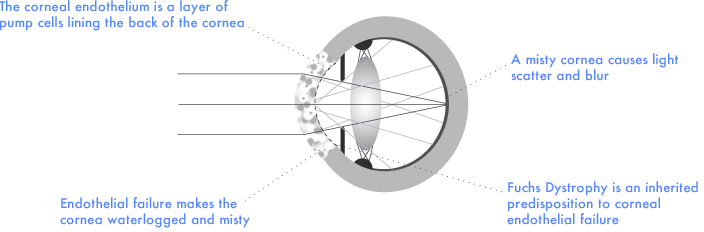
The commonest cause of loss of corneal transparency is failure of the delicate pump cell layer lining the back of the cornea (the corneal endothelium). This may occur as a consequence of other eye operations, or because of a common inherited predisposition to corneal endothelial failure called Fuchs dystrophy. Selective replacement of the damaged endothelial layer (endothelial keratoplasty) in an operation similar to modern cataract surgery has superseded full thickness transplantation (penetrating keratoplasty) in the treatment of endothelial failure. Advantages of this minimally invasive approach are surgery improved vision and a faster visual recovery.
Transplant and non-transplant treatments for kerataconus
Keratoconusis a common, treatable cause of impaired vision in young people characterised by progressive steepening and irregularity of the corneal shape.
The aim in modern keratoconus treatment is to stabilise corneal shape and prevent further visual impairment using a treatment called collagen cross-linking (CXL). Implants (ICL, ICRS) and laser treatment (TransPRK) can be used in tandem with CXL to restore better vision in many cases, reducing dependence on contact lenses.
Non-transplant treatments for keratoconus are relatively new, and are only now becoming routinely funded for NHS patients. For patients who already have more advanced keratoconus, corneal transplantation is still the best way to restore a more normal corneal shape and improved vision. The corneal endothelial layer is normal in patients with keratoconus, and this layer is the main target for rejection reactions in corneal transplantation. The aim in modern transplantation for keratoconus patients is therefore to leave delicate endothelial layer at the back of the cornea in place, and to replace the abnormally shaped corneal tissue in front. This operation called Deep Anterior Lamellar Keratoplasty (DALK).